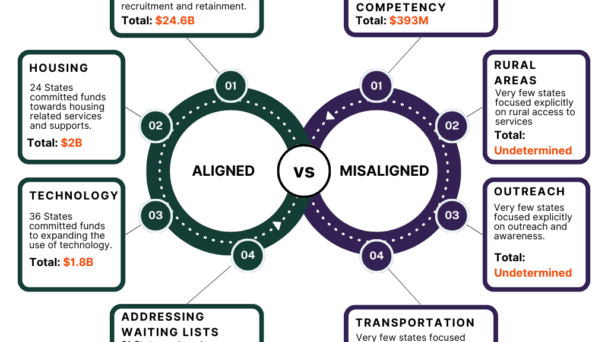
Did ARPA Investments in Home and Community-Based Services Reach Those Who Needed it Most?
Every year, millions of people choose to live independently and receive care services in their homes and communities; opting for this over moving to a care facility or institution. For…